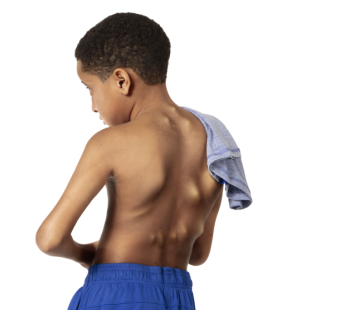
Over half of patients with FOP are initially misdiagnosed1,2
International Fibrodysplasia Ossificans Progressiva Association (IFOPA) registry data demonstrate that 52.5% of patients with FOP initially receive an inappropriate diagnosis.1,2*
FOP is often misdiagnosed with common misdiagnoses, including cancer,
juvenile hyaline fibromatosis![]() ,
,
Juvenile fibromatosis is a rare, autosomal-recessive disease characterized by papulonodular skin lesions, gingival hyperplasia, decreased joint mobility and bone involvement in variable degrees.9
myositis ossificans traumatica![]() ,
,
The formation of ectopic bone inside muscles and other soft tissue after a traumatic injury to the area. This injury is usually the result of repeated muscular trauma.10
and Klippel-Feil Syndrome![]() .
.
1,2
A rare disease characterized by congenital cervical fusion. Other symptoms vary between patients and may affect a range of organ systems.11
*From a total of 299 patients surveyed.
Patients with FOP see on average 3.3 physicians before receiving a correct diagnosis1
Delay in diagnosis is approximately 1.5 years1
Unfortunately, many patients with FOP undergo unnecessary diagnostic and therapeutic interventions that can lead to long-term harm.3
Results from a questionnaire sent to patients with FOP (N=138) found:3

67%
of patients underwent invasive procedures for diagnosis that can exacerbate heterotopic ossification (HO)
Disclaimer: These recommendations are not the complete guidelines. Please refer to the ICC website to download the full guidance.
Go feet first!
FOP should be suspected if patient presents with bilateral great toe malformation and tumor-like soft-tissue swellings.3
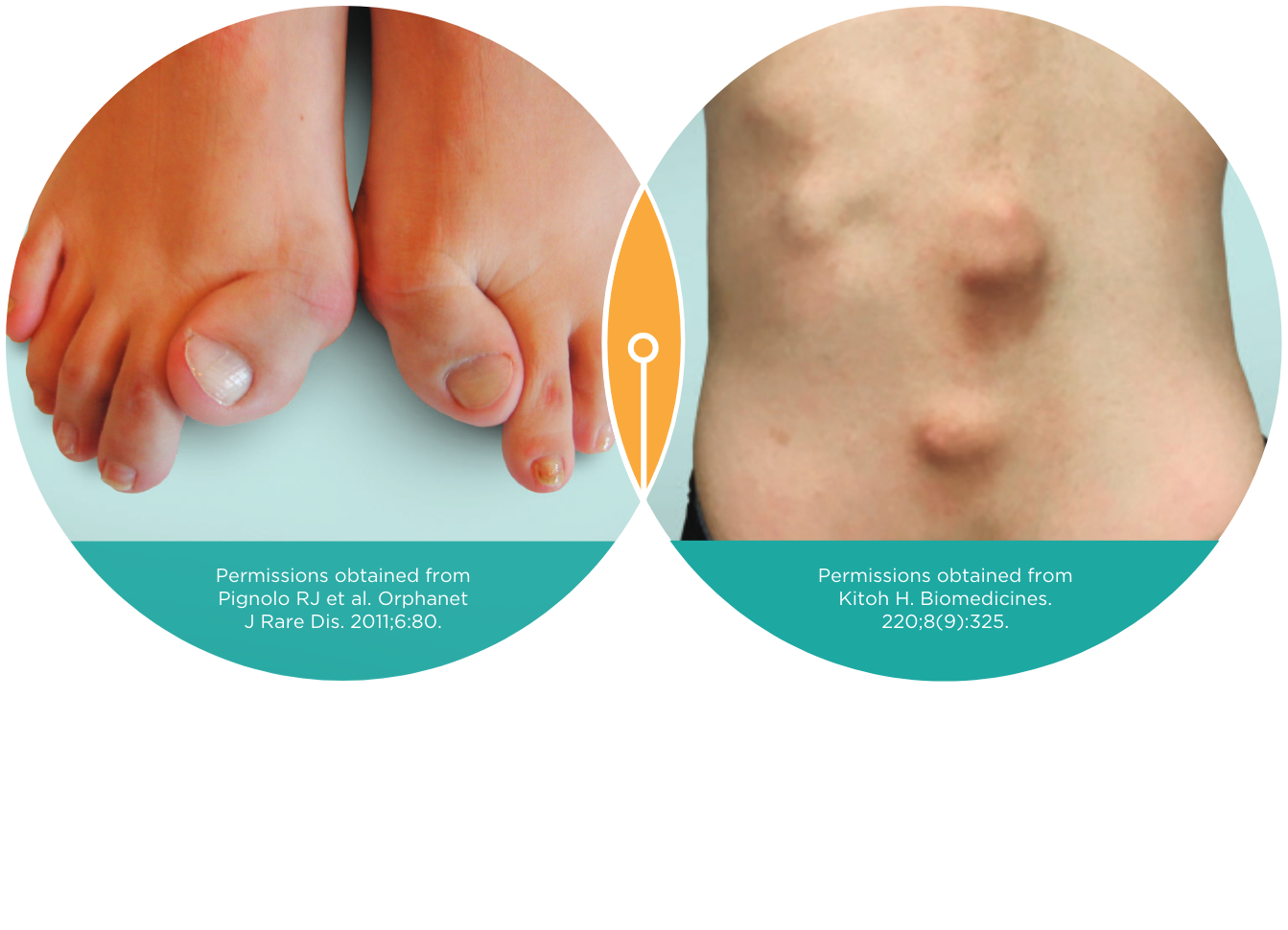

Diagnosis is clinical but genetic testing for mutation in the ALK2/ACVR1 gene can also be used to confirm the diagnosis3–5
Signs and symptoms to look out for:3,6
•Malformation of great toes
•Tissue swelling
•Scalp nodules (in infants)
•Lumps on the neck and back
•HO
Due to the symptoms of FOP, patients may be seen by a range of healthcare professionals (HCPs), including endocrinologists, orthopedists and rheumatologists, before receiving an accurate diagnosis of FOP.7–9 It is important that these HCPs are aware of the signs and complications of FOP in order to make a prompt diagnosis and avoid iatrogenic harm.3,5
Genetic counselors may also be provided for patients to discuss concerns regarding family planning.5
1. Sherman LA et al. Presented at ASBMR 2020; Virtual Event: September 11–15 2020. 2. Sherman LA et al. abstract P841. J Bone Miner Res 2020;35(Suppl 1):1–337. 3. Kitterman JA et al. Pediatrics 2005;116:e654–e66. 4. Di Rocco M et al. Orphanet J Rare Dis 2017;12:110. 5. Kaplan FS et al. Proc Intl Clin Council FOP 2022;1:2–127. 6. Piram M et al. J Am Acad Dermatol 2011;64:97–101. 7. Kannu P and Levy CE. J Peds 2021;232S:S3–S8. 8. Shi X et al. Medicine (Baltimore) 2020;99:e19933. 9. Hsiao E et al. Endocrine Abstracts 2020;70:AEP1025.
10. Braizat O et al. Cureus 2020;12:e10823. 11. Hanisch M et al. Head Face Med 2018;14:23. 12. Tracy MR et al. Clin Orthop Relat Res 2004:183-190.